Caring for Caregivers During
COVID-19 Crisis & Beyond
by Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com and
Contributing Writers: Samantha Shune, PhD, CCC-SLP &
Ashwini Namasivayam-MacDonald, PhD, SLP(C), CCC-SLP, Reg. CASLPO

How do caregivers (aka, carers or care partners) stay calm, patient, and engaged during this COVID-19 crisis? It is time to care for our caregivers too.
Time for Joy & Time for Hard Questions
Hospitals around the world play inspirational songs of joy and encouragement every time a person with COVID-19 is discharged. The following are examples of songs that have been played over intercoms: “Sweet Caroline,” by Neil Diamond here in Boston-Red Sox Nation (sorry New York City!); “Beautiful Day,” by U2; and “Gonna Fly Now,” by Bill Conti — better known as the Rocky Theme. Tears come to my eyes every time I watch videos of people wheeling down hospital corridors to these songs through the lines of hospital staff clapping.
Now we have to ask the hard questions:
- Were the discharge options limited during that person’s discharge planning?
- As some nursing homes are not accepting people from the hospital with COVID-19, are many people being discharged home to unpaid family/friend caregivers?
NOTE: I will use the term caregivers throughout, as that is the term most often used in research and in healthcare. However, consider other terms, such as: carers and care partners, as these avoid the connotation that this is only a one-way relationship of a giver and a receiver.
- Are these caregivers prepared? Do they accept the potentially new role? Are they equipped with the supplies, devices and PPE? Have they been trained to address the person’s many rehabilitation needs? What if the person had post-extubation dysphagia (see prior blog)? After all, we used to have family members come into the hospital or rehabilitation center for in-person caregiver trainings prior to a discharge home.
- What about caregivers of people who have been at home with or without COVID-19? Have they been putting off the health care needs for themselves and the person they care for? Have they had questions answered via telehealth? Have they been able to still receive necessary supplies (e.g., for people with chronic tracheostomies — see prior blog for trach resources.)
- Are caregivers of people with difficulty swallowing (dysphagia) having increased challenges due to minimal outpatient services available?
- Did you know that Medicare/CMS still has NOT approved payment for dysphagia telehealth services provided by speech-language pathologists who specialize in swallowing! They only approved speech, language and voice evaluations and treatments.
- Here is a list of Medicare’s temporarily approved telehealth codes: Telehealth Services for PHE for the COVID-19 pandemic effective March 1 2020-updated April 30 2020.
- Here is an article by the American Speech-Language Hearing Association on advocacy needed for Telehealth.
–> Therefore, these caregivers of individuals with difficulty swallowing (dysphagia) may be particularly struggling!
Take a Moment to Thank Our Caregivers:
Before we get into statistics around caregivers in the United States, let us think about the sacrifices that are made every day by caregivers around the world. The song “Rise Up,” by Andra Day encourages caregivers to push through the hard times and find those moments of joy and connectedness! We are all struggling through these stressful times, and the in-home caregivers will likely be needing extensive support from the healthcare community, as well as from other family and friends right now!
Caring for Caregivers – Statistics & Research
Caregivers across the United States have really been taking the burden off our healthcare system, even before this COVID-19 pandemic hit. Per the AARP in 2013, 40 million family caregivers were volunteering 37 billion unpaid hours to care for adults who require assistance in their homes. That contribution to society was equal to $470 billion dollars. Per the National Alliance for Caregiving (NAC) & AARP’s Public Policy Institute report from 2015, the number rose to 43.5 million American caregivers with the contribution exceeding $500 billion! Imagine how the numbers will continue to rise with the COVID-19 pandemic and with the baby boomer population. (See this link for many statistics around caregiving at Caregiver.org). That 2015 NAC & AARP report noted that 1 in 4 caregivers spends 41 hours or more providing necessary assistance.
People may be picturing all these caregivers as older (i.e., spouses and adult-children in their 50’s-60’s+ caring for their parents). Even Riffin and colleagues in 2019 found the average age of caregivers was 57.1. However, per AARP in 2018, 1 in 4 caregivers were millennials! Additionally, per a poll by The Associated Press-NORC Center for Public Affairs, as described here on AARP.org, these younger caregivers were more likely to experience caregiver burden.
- 80% of younger caregivers rated their responsibilities as “moderately stressful.”
- Whereas, 67% of the older caregivers rated the stress as moderate.
Prolonged stress and caregiver burden can have a serious impact.
The speech-language pathologist, Lisa Milliken, MA, CCC-SLP, FNAP, CDP (in her MedbridgeEducation webinar – see more info under resources below) advised to not underestimate prolonged stress. It is a real physiological risk.
“We want caregivers to know this,” Milliken stated.
Milliken’s webinar recommended a host of strategies to ease the strain, such as: laughter, mindfulness, checklists, healthy eating/sleeping habits, keeping a journal, talking with friends, meditation, visualization, breathing and progressive relaxation exercises, and certainly movement/exercise. Blumenthal, et al. (2012) found that high energy/aerobic exercise for 30-45 minutes 3-5 times a week was most effective in reducing depressive symptoms (compared with low impact and less often). Above all, Milliken advised to recognize your symptoms and seek professional help as needed.
Zarit (2006) summarized that up to 70% of caregivers show some significant signs and symptoms of depression, with 25-50% of these caregivers being clinically depressed. Riffin and colleagues (2019) took a national sample of unpaid caregivers and noted:
- 21% self-reported poor physical health,
- 13% reported depression,
- 13% reported anxiety, and
- few received supportive services (e.g., 7% had caregiver training, 10.4% benefited from respite care, and only 4.4% used support groups).
- Fortunately, according to the Riffin sample, 70.4% reported receiving help from family and friends, but
- 56.1% still felt a caregiver burden.
This caregiver burden increases when the care recipient has difficulty swallowing (dysphagia). Nund and colleagues (2014) from Australia performed a qualitative study, which categorized the caregivers’ experiences with people who received curative and non-surgical treatment for head and neck cancer. Their comments from interviews were organized into these 4 themes:
- Dysphagia disrupts daily life. (Example: “Meal preparation takes more time and effort.”)
- Carers make adjustments to adapt to their partner’s dysphagia. (Examples: ‘We [don’t] sit at the table…there is less talk… less other things happening…because we don’t want to go anywhere because he can’t eat.” and ‘‘You have to live with the new life…and the new life is that meal preparation is different from anybody else’s or different from what it used to be.”)
- Disconnect between carers’ expectations and the reality of dysphagia.
- Experiences of dysphagia-related services and informal supports. (Example, “Once treatment is over, you are cast off to sail alone. It is very lonely, fearful and frustrating time.”)
Nund, et al. reminded speech-language pathologists (SLPs) that caregiver supports/training need to be clear, well-organized, understandable, personalized, and NOT in medical jargon/terminology. Otherwise, the caregivers are not going to reach out for more support.
Oldenkamp and colleagues (2016) compared spousal burden and adult-child caregiver burden. Spousal burden was subjectively higher overall when compared to the adult-child caregivers, as the spouses reported more of their own mental and physical health issues. Is that due in part to the older age of the spouses and their prior medical issues? For both groups, the following 2 factors predicted higher burden over time: poor health status of the care recipient and the amount of time required/invested in caregiving. Imagine when a person has difficulty swallowing and is at risk for aspiration pneumonia and/or choking. Additional time is required to prepare meals and potentially feed that individual slowly with specific safer swallowing strategies outlined by the SLP.
Therefore, it makes sense that dysphagia researchers, Namasivayam-MacDonald & Shune, found that dysphagia was an independent predictor of physical and emotional caregiver burden in their 2019 study. Here are some findings from their studies from 2018 to 2020:
- 40% of these caregivers of people who have dysphagia reported their physical and emotional burden was moderate to severe (2019).
- In a follow-up study, Shune & Namasivayam-MacDonald (2020) found when the care recipient had dysphagia, the caregiver had over 2 times greater odds to have emotional burden (OR = 2.06).
- 70% of spousal caregivers of older adults with dysphagia reported moderate-severe emotional burden (2020).
- This burden seems to increase further when the care recipient has advanced dementia and a feeding tube. In a systematic review by Namasivayam-MacDonald and Shune (2018), they highlighted a Bentur, et al. (2015) study from Israel. This showed that 75% of caregivers who manage feeding tubes reported “heavy” to “very heavy” burden of care. (This is quite high when compared with when no tube feeding was involved. Only 19% of those caregivers reported a heavy to very heavy burden.)
Namasivayam-MacDonald and Shune (2018) urged dysphagia researchers to study caregiver burden further due to a “paucity of evidence” on how and why dysphagia impacts the caregivers. They noted a common theme in people recovering from head and neck cancer: “negotiating a new normal,” but stated that a “new normal” is unfortunately not always achievable in the population of older or very old adults who may be dealing with chronic and progressive diseases/disorders.
My last question is: how does this caregiver burden interact with the care recipient’s own burdens?
The person who has difficulty swallowing may have their own challenges from the change to their health and quality of life. Ekberg and fellow researchers (2002) surveyed people with dysphagia and found:
- Over 50% reported to eat less.
- 44% lost weight in prior 12 months.
- 33% still feel hungry and thirsty after their meal.
- 84% said that eating should be enjoyable, but only 45% still found it to be enjoyable.
- 41% report anxiety with mealtimes.
- 36% avoid eating with others due to the dysphagia.
*******
Read More from Doctors
Ashwini Namasivayam-MacDonald &
Samantha Shune
First, from Ashwini Namasivayam-MacDonald, PhD, SLP(C), CCC-SLP, Reg. CASLPO:
Caregiver Burden & Caring for Caregivers
Everyone experiences burden differently. However, our research has demonstrated the following factors and patterns:
- Spousal caregivers of older adults with dysphagia are more likely to experience emotional burden, whereas
- Caregivers of aging parents with dysphagia are more likely to experience both emotional and physical burdens. This is likely due to the fact that these adult children of aging parents are balancing jobs and their own family responsibilities.
- Caregivers who are female are more likely to feel burdened.
- Caregivers who have their own health issues are also more likely to feel the burden.
- Family conflict regarding how to take care of the care recipient heightens the burden.
While some of these factors are unavoidable, I think it is crucially important that the caregivers seek support for their own health issues so those do not further contribute to their burden.
More Tips on How Caregivers Can Reduce the Burden:
- Caregivers should not hesitate to seek professional support if needed. If they are feeling overwhelmed, they should speak to their primary care physician about a referral to a social worker, counsellor, and/or psychologist who may be able to help work through some of their emotions and offer resources.
- Caregivers should not hesitate to ask clinicians (and all related healthcare providers) for support when it’s needed. For example, if there’s something they don’t understand or feel would be better digested in a written format, they should ask the clinician for clarification and/or for a copy of the written report and recommendations. Caregivers should also ask for resources to help guide the interventions that they have been asked to help implement.
- General caregiver burden research has also demonstrated that caregivers benefit from support from their social networks. As such, it is important that caregivers connect with family and friends outside of the home (either by phone or videoconferencing) during this challenging time.
Second, from Samantha Shune, PhD, CCC-SLP:
Why is Dysphagia an Independent Predictor of Caregiver Burden
Swallowing and eating do not happen in isolation, so we cannot possibly treat them in isolation! The therapist cannot step in and advise on what is the best and safest way to swallow without considering all the psychosocial issues around eating and swallowing. Additionally, healthcare providers have to realize that this dysphagia may be only one issue that the person and caregiver are trying to manage among many medical and emotional burdens. Are we putting too much on their plates?
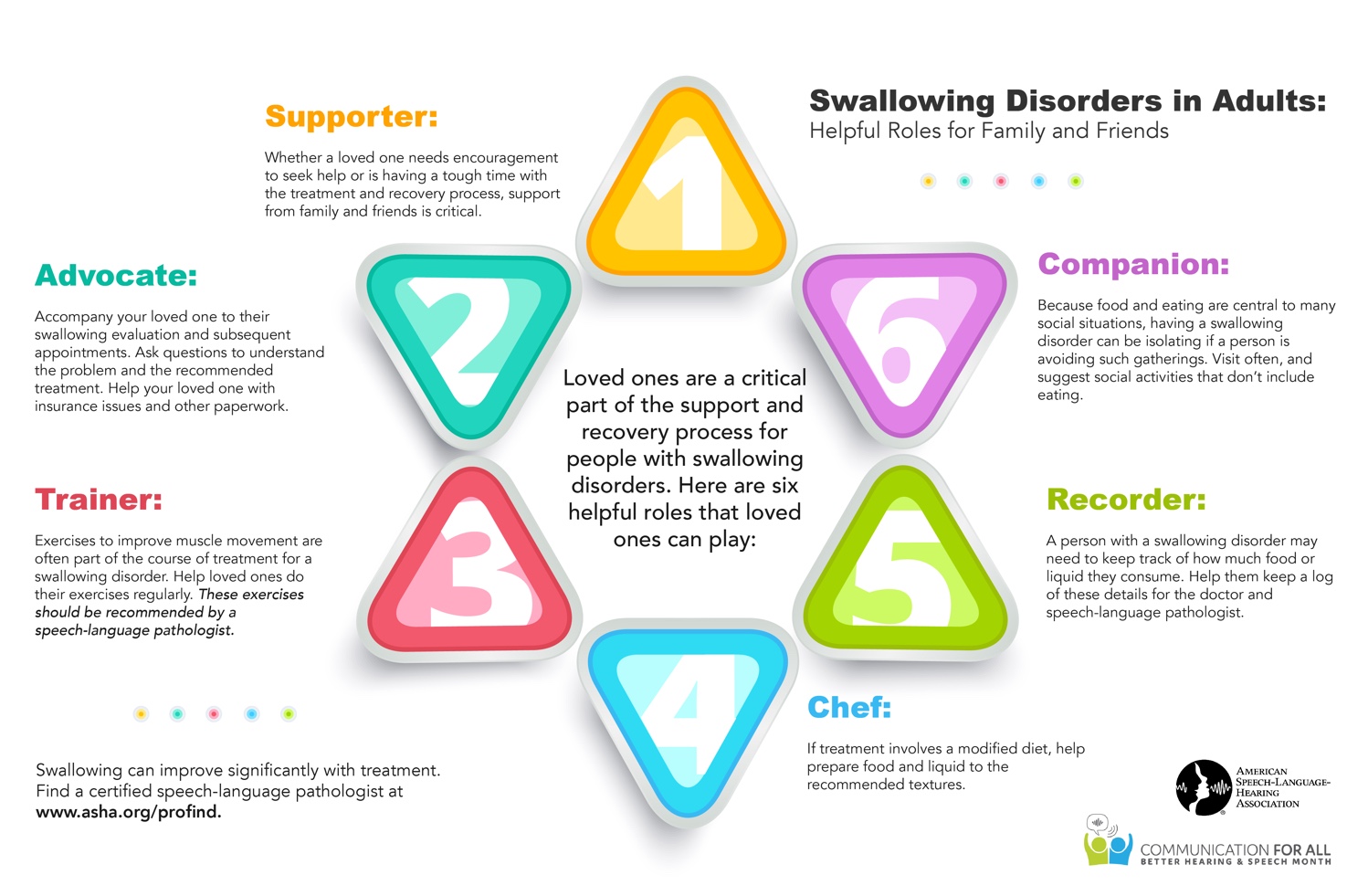
American Speech-Language Hearing Association Infographic from 2019 Better Hearing & Speech Month. Shows “helpful roles” for caregivers of adults who have difficulty swallowing (dysphagia). There are already 6 roles they need to perform, and that is in addition to other daily caregiving needs. We need caring for caregivers!
While dysphagia has been shown to be an independent predictor of caregiver burden in some populations (e.g., older adults), we are not entirely sure yet why the dysphagia increases burden. Previous literature, though, provides some suggestions, including:
Logistics-related tasks, such as an increased financial strain and the following:
- grocery or online shopping for specific food, drink, supplement items for the individual with dysphagia,
- potentially increased costs associated with those specific items,
- preparing separate meals, and
- the rigid schedule and tasks associated with tube feeding.
Psychosocial “events” and feelings, such as:
- not being able to eat out with friends or attend other significant social events (and maybe not even getting invited to those events),
- feeling guilty about eating foods that the person with dysphagia cannot eat,
- feeling guilty over trying to withhold foods from the person with dysphagia,
- increased fear and anxiety during mealtimes (e.g., concerns regarding aspiration and will my loved one start choking).
I have discovered a clear theme, based on some of my ongoing qualitative research (an interview study that was going to be presented as a poster at the Dysphagia Research Society Annual Meeting that was cancelled due to COVID-19):
—> Dysphagia is a chronic condition experienced by both the individual with dysphagia AND their family. There is a loss of socialization and pleasure associated with eating. Eating becomes an activity primarily for nutrition. Ultimately, adaptation to the illness requires readjustment of a family’s definition of normalcy and learning to cope with the negative emotions associated with the disease (which may differ across different members of the family).
We found in our study that families often need support and training in order to overcome the barriers to healthy adaptation to the illness they were experiencing (in this study’s case – stroke and dysphagia). As listed above, some of these barriers were more logistic in nature. Therefore, the SLP could train these task-specific dysphagia-related activities. Whereas other barriers were more psychological (e.g., related to coping mechanisms, high anxiety or depression), and those would require additional resources and appropriate referrals to pyschologists and/or social workers.
How Speech-Language Pathologists (and the medical team) Can Care for Caregivers of People with Dysphagia:
- We need to identify dysphagia early, allowing us to then intervene with caregivers earlier and attempt to reduce the burden before it becomes unmanageable.
- We need to engage caregivers in conversation. Ask them how they are doing and what their needs are. We need to ask them right from the beginning if they are feeling capable in this caregiving role. If not, think about ways we can increase self-efficacy and help identify additional or alternative support people.
- We should avoid the use of highly medicalized language.
- We should also be careful not to assume that a family member/loved one is willing and/or able to take on the caregiving role.
- When we explore what goals are important for the person who has difficulty swallowing, we need to include the caregivers in the creation of these goals for therapy.
- Provide education to both the person with dysphagia and the caregiver (ideally in multiple modalities). We need to be careful not to bombard the caregivers with so much information, and we should always avoid using medical jargon.
- We should be aware of mental health counseling services and other resources in our area and provide referrals when appropriate. We should be a bridge to these other services.
*******
*******
Summary of Caring for Caregivers
Times are changing. This was already the case with the baby boomers coming into older ages, and now with the effects of COVID-19, we may not be prepared with enough caregivers! Research from the University of Michigan by Ryan and colleagues (2012) forecasted:
“Between 2010 and 2030 the number of 75-year-olds without a living spouse to provide care could double to 1.8 million. Those without an adult-child nearby could increase by a multiple of six, to more than 600,000 by 2030.”
These numbers in addition to the emotional and physical burdens of caregiving may seem overwhelming. It takes federal and local governments, community resources, and healthcare institutions to support those who provide all these volunteer hours. The medical team, including the speech-language pathologist, plays a crucial role in treating the whole person who has difficulty swallowing (dysphagia). We must take care of the caregivers (as listed in tips above).
Caregiving is not a one-way street from giving to receiving. These support systems should help ease the burden. Then these family caregivers can have more opportunities for the joy and the reciprocal connection that comes with caring for loved ones.
*******
RESOURCES FOR CAREGIVERS & CLINICIANS
Please use the comment section below to add your own resource ideas and how you have been coping before and during this COVID-19 pandemic.
Please check out Dr Shune’s 2019 NFOSD Webinar (along with Michele Vandehey):
Webinar Recording: Dysphagia’s Broader Impacts on Caregivers & Families
Other Caring for Caregivers Resources (in no particular order):
Updated 11/13/20
- CARES Screening Tool by Shune, S.E., Resnick, B., Zarit, S.H. & Namasivayam-MacDonald, A.M. (November, 2020). Creation and Initial Validation of the Caregiver Analysis of Reported Experiences with Swallowing Disorders (CARES) Screening Tool. American Journal of Speech-Language Pathology, 29, 2131-2144. https://doi.org/10.1044/2020_AJSLP-20-00148
- Family Caregiver Alliance (FCA) (that is Caregiver.org)
- National Alliance for Caregiving (that is Caregiving.org)
- NFOSD Online Support Groups & all articles/resources under the “Patients & Caregivers” Section.
- Varindani-Desai, R. (2017). Caregiver’s Guide to Dysphagia in Dementia at
https://swallowingdisorderfoundation.com/caregivers-guide-dysphagia-dementia/
- Varindani-Desai, R. (2017). Caregiver’s Guide to Dysphagia in Dementia at
- National Institute on Aging (NIA) resources for caregivers: https://www.nia.nih.gov/health/caregiving
- Caring Across Generations: https://caringacross.org/why-care/
- American Association of Caregiving Youth: https://www.aacy.org
- Hilarity For Charity (HFC): I love this – they bring light and humor to support people with Alzheimer’s & Dementia.
- COVID-19 Resources for Alzheimer’s & Dementia Caregivers: https://wearehfc.org/programs/covidsupport/
- ARCH National Respite Network:
- 9 Steps to Respite – Family Fact Sheets: https://archrespite.org/consumer-information/family-caregiver-fact-sheets
- COVID-19 Info for Caregivers
- Hormel Health Labs: https://www.hormelhealthlabs.com/resources/covid-19-resource-faq/
- Ordering Thickened Liquids – Clear – Gum-based (not corn-starch) Use Coupon Code EASY5 for $5 off. Sugar-free Peach Mango is really good!!
- Ordering Purees (ready to eat). Use Coupon Code PUREE15 for discount.
- (I do not receive any financial incentives here; passing along savings!)
- Caregiver Action Network (CAN): https://caregiveraction.org/covid-19
- AARP – nursing home transfers: https://www.aarp.org/caregiving/health/info-2020/coronavirus-transfers-to-nursing-homes.html
- Rosalynn Carter Institute for Caregiving: https://www.rosalynncarter.org
- Elizabeth Dole Foundation: https://hiddenheroes.org/coronavirus/
- For caregivers of children with pediatric feeding disorders, please see: FeedingMatters.org
- Book: Meditations for Caregivers by Barry J. Jacobs Psy.D., Julia L. Mayer Psy.D. https://www.aarp.org/entertainment/books/bookstore/home-family-caregiving/info-2016/meditations-for-caregivers.html
- Online Guide: A Caregiver’s Guide for Family and Loved Ones
https://www.premiernursingacademy.org/ resources/family-caregivers- support - Family-Centered Design National Report, https://www.caregiving.org/wp-content/uploads/2019/05/NAC_LEAD-Coalition_Paving-the-Path_Report_May-2019.pdf, notes:
- “the demand for family caregivers is growing exponentially, while the supply is shrinking” (p. 8).
- “The demand for caregivers is fast outstripping the available supply. We must build a pathway for friends and relatives to provide care without sacrificing their own quality of life and that better recognizes and values their unique perspectives, always protecting the patient’s autonomy and voice. Improving the care that people living with illness or disability receive depends on it” (p.2).
- I recommend this course by Lisa Milliken, MA, CCC-SLP, FNAP, CDP
on MedbridgeEducation so that SLPs can help guide caregivers through stressful times. The Clinician’s Role in Helping to Manage Family Caregiver Stress: https://www.medbridgeeducation.com/courses/details/the-clinicians-role-helping-manage-family-caregiver-stress-lisa-milliken. (If you have not become a member of Medbridge yet, consider using the coupon code “SWALLOWstudy” at checkout to support my website/blogs. I am an affiliate member with Medbridge to pass on discounts to you, and I receive a very small commission. Thank you). - More information/resources for clinicians on Dysphagia Telehealth from Purdue University’s I-EaT Lab. Please see complete details on website, but here are some helpful links to pdfs:
- Read more about:
- Dysphagia diets (International Dysphagia Diet Standardization Initiative/IDDSI.org) and
- Food preparation (dysphagia diet recipes according to IDDSI)
- Why Puree?,
- More on Pureed & Liquidised foods, as well as product reviews/discounts and
- Thickened liquids (with ideas for nutritious and thicker smoothies).
*******
Thank you to my guest bloggers:
Samantha Shune, PhD, CCC-SLP is an assistant professor in the Communication Disorders and Sciences Program at the University of Oregon. Her research and clinical interests include the effects of healthy and pathologic aging on swallowing and the mealtime process. She is particularly interested in better understanding shared food-related activities as opportunities to therapeutically target improved quality of life for both older adults and their social networks (e.g., partners, family members). In addition to her research, she currently teaches in the area of medical speech-language pathology and organizes a swallowing disorders support group. More information about her work is available at https://eatinglab.uoregon.
See Dr Shune’s prior blog on SwallowStudy.com: Mealtime Success: From the Table to the Stomach
AND
*******
REFERENCES for Caring for Caregivers
AARP (2015). Retrieved from: https://www.aarp.org/ppi/info-2015/caregiving-in-the-united-states-2015.html
Bentur N., Sternberg S., Shuldiner J., Dwolatzky T. Feeding tubes for older people with advanced dementia living in the community in Israel. Am. J. Alzheimers Dis. Demen. 2015;30:165–172. doi: 10.1177/1533317514539726.
Blumenthal, J. A., Smith, P. J., & Hoffman, B. M. (2012). Is Exercise a Viable Treatment for Depression?ACSM’s health & fitness journal, 16(4), 14–21. https://doi.org/10.1249/01.FIT.0000416000.09526.eb https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3674785/
Ekberg, O., Hamdy, S., Woisard, V. et al. (2002). Social and Psychological Burden of Dysphagia: Its Impact on Diagnosis and Treatment. Dysphagia 17, 139–146. https://doi.org/10.1007/s00455-001-0113-5 https://link.springer.com/content/pdf/10.1007/s00455-001-0113-5.pdf
Milliken, L. (n.d.). The Clinician’s Role in Helping to Manage Family Caregiver Stress [Webinar]. In Medbridge Education. Retrieved from https://www.medbridgeeducation.com/courses/details/the-clinicians-role-helping-manage-family-caregiver-stress-lisa-milliken
Namasivayam-MacDonald, A.M. & Shune, S.E. (2018). The Burden of Dysphagia on Family Caregivers of the Elderly: A Systematic Review. Geriatrics. 3(2), 30. https://doi.org/10.3390/geriatrics3020030 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6319247/
Namasivayam-MacDonald, A. & Shune, S. (2019). The influence of swallowing impairments as an independent risk factor for burden among caregivers of aging parents: A cross-sectional study. Geriatric Nursing. Advance online publication. https://doi:10.1016/j.gerinurse.2019.06.008
National Alliance for Caregiving (NAC) and AARP Public Policy Institute. (2015). Caregiving in the U.S. Retrieved from
https://www.aarp.org/ppi/info-2015/caregiving-in-the-united-states-2015.html and
https://www.caregiver.org/caregiver-statistics-demographics
Nund, R.L., Ward, E.C., Scarinci, N., Cartmill, B., Kuipers, P., & Porceddu, S.V. (2014). Carers’ Experiences of Dysphagia in People Treated for Head and Neck Cancer: A Qualitative Study. Dysphagia, 29, 450-458. https://link.springer.com/content/pdf/10.1007/s00455-014-9527-8.pdf
Oldenkamp M, Hagedoorn M, Slaets J, Stolk R, Wittek R, Smidt N. (2016). Subjective burden among spousal and adult-child informal caregivers of older adults: Results from a longitudinal cohort study. BMC Geriatr., 16(1), 208. doi:10.1186/s12877-016-0387-y. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5142272/
Riffin, C., Van Ness, P. H., Wolff, J. L., & Fried, T. (2019). Multifactorial Examination of Caregiver Burden in a National Sample of Family and Unpaid Caregivers. Journal of the American Geriatrics Society, 67(2), 277–283. https://doi.org/10.1111/jgs.15664. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6367031/
Ryan, L.H., Smith, J., Antonucci, T.C., Jackson, J.S. (2012). Cohort differences in the availability of informal caregivers: Are the Boomers at risk? Gerontologist, 52(2), 177-88.
Shune SE, Namasivayam-MacDonald AM. (2020). Swallowing Impairments Increase Emotional Burden in Spousal Caregivers of Older Adults. J Appl Gerontol., 39(2), 172‐180. doi:10.1177/0733464818821787.
https://pubmed.ncbi.nlm.nih.gov/30623709/
Zarit, S. (2006). Assessment of Family Caregivers: A Research Perspective. In Family Caregiver Alliance (Eds.), Caregiver Assessment: Voices and Views from the Field. Report from a National Consensus Development Conference (Vol. II) (pp. 12 – 37). San Francisco: Family Caregiver Alliance.

