DRS Digest 2024: Why DRS
by Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com

Introduction to Why DRS
Almost 400 people gathered in San Juan Puerto Rico this March from 22 different countries across and many different disciplines (e.g., basic scientists, dietitians, dentists, engineers, speech-language pathologists, occupational therapists, and pediatric through adult physicians across related specialties)! This conference truly reinforced why I attend the Dysphagia Research Society (DRS) meetings every year. In this Dysphagia Digest, I want to share my top reasons Why DRS has had such an impact on my career as a medical speech pathologist who specializes in swallowing and swallowing disorders (dysphagia). DRS – as an organization and their annual conference – is for clinicians, professors/researchers, scientists, and industry partners. We are all in this together for the benefit of people with difficulty swallowing (dysphagia) and to advance the science of swallowing and swallowing disorders.
Of course, I got immediately carried away with my Reason #1 of Why DRS while still pondering other reasons. Therefore, in true SwallowStudy.com style, I will take a deep dive in this blog into the #1 reason, but here is a look at my Top 10 Why DRS (aka, reasons to attend annual conferences of the Dysphagia Research Society / DRS):
- Making you question everything
- Supporting new investigators & all those new to the dysphagia field
- Networking
- Interdisciplinary connections
- Providing swallow solutions that can be applied immediately
- New discoveries
- Advocating for public health
- Showing you recent research that you might have missed in your busy clinical day
- Highlighting the importance of comprehensive dysphagia evaluation and management across disciplines, getting you out of your own disciplines’ silo
- Does partying, dancing, eating, and schmoozing count under Networking? I would state that these deserve their own place in the list!
The learning can continue through affordable options from DRS, such as the DRS Webinar Series — formerly known as the Dysphagia Research Society Institute for Education (DRSIE)
- See the DRS Webinar Series page. This updates often and contains the library of prior DRSIE’s free monthly webinars for DRS members ($50 for non-members). These older webinars are no longer available for continuing education credit.
Since continuing education is so important, here are just a few other no-cost to low-cost options:
- Dr. Thibeault reminded the audience of the free expert lectures from the University of Wisconsin available for ASHA CEUs on their website: https://cme.surgery.wisc.edu/courses/voice
- The American Board of Swallowing and Swallowing Disorders (AB-SSD) offers:
- Affordable Intermediate and advanced CEUs: https://www.swallowingdisorders.org/page/courses
- Free CEUs thanks to a grant from Bracco: https://www.swallowingdisorders.org/page/braccoce
- Special thanks to the National Foundation of Swallowing Disorders (NFOSD) for providing content for people with dysphagia, their caregivers, as well as healthcare providers (See Resources Tab). While these do not tend to provide continuing education credits, the learning is extremely valuable.
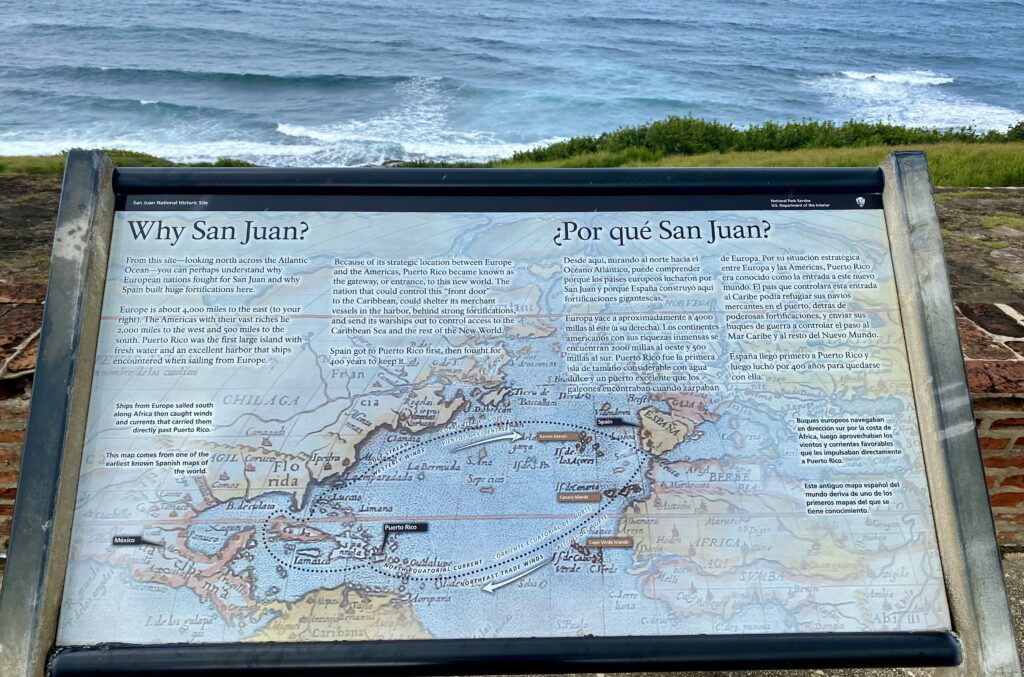
This sign in Old San Juan does not ask Why DRS, but it does ask: “Why San Juan?” Of course conference goers did not ask why we were in such a beautiful location for DRS2024. We can thank Dr. Susan Langmore, who was the DRS president in the 2019-2020 year when she planned Puerto Rico for our Spring conference, which was sadly cancelled due to the onset of the COVID pandemic. We finally made it!
Now for my Why DRS Reason #1…
DRS Makes Us Question What We Think We Know
Questioning is essential to staying up-to-date and applying critical thinking skills to each research article, each person we serve, and each practice pattern. This #1 Why DRS uses the example of SENSATION.
Sensation in Swallowing & Airway Protection
And… No, not the sensation of digging your toes into the sand after a full day of stimulating conference sessions! Rather, the fact that there is still so much to learn about sensation within the field of swallowing and swallowing disorders (dysphagia). There is so much more research that needs to be done. DRS motivates us to do more and always ask: “What else?” – as Joan Arvedson, PhD, CCC-SLP says.
As we know, the swallow is so complex, as is the larynx itself, which is tasked with breathing, voicing, and airway protection when swallowing and against aspiration and/or refluxed contents. In the field of dysphagia, we often say good sensory input is needed to trigger good motor output, due to the complex sequence of events that is normal swallowing.
Many clinicians know that the Superior Laryngeal Nerve (SLN) provides sensory input to the larynx, but that is about it. We really investigated this deeper at the DRS pre-conference sessions on March 12, 2024 on laryngeal reflexes across the lifespan. Speakers were: Dr. Susan Thibeault, PhD, CCC-SLP, Dr. Greg R Dion, MD, FACS, and Dr. Jesse Hoffmeister, PhD, CCC-SLP. This session was a highlight of the week.
Dr. Susan Thibeault, PhD, CCC-SLP from the Division of Otolaryngology-Head and Neck Surgery, University of Wisconsin – Madison shared her research regarding the importance of sensory receptors of the pharynx and larynx for reflexive airway protection. She educated on mucosal mechanoreceptors that monitor sensation via the Vagus nerve and this cranial nerve X’s internal branch of the superior laryngeal nerve or iSLN (which in turn has three branches: superior, middle, and inferior). The iSLN carries sensory/afferent information to the nucleus tractus solitarius (NTS) of the lateral medulla in the brainstem. Dr. Thibeault referred to her research with Dr. Alexander Foote (2021 & 2022) to show how these afferent nerves (sensory branches for mechanical, chemical, and thermal sensations) have a specific pattern of location across the pharynx, supraglottic larynx, vocal cords, and subglottic larynx. This information is essential to our understanding of the results of our comprehensive swallowing evaluations and to our guiding of targeted treatments.
It is important to first go to their 2021 review article to see Figures 1 & 2 that display the internal branch of the superior laryngeal nerve (iSLN) and its superior, middle, and inferior branches. Do you know what parts of the mucosa are covered by each branch (see Figure 1)?
Superior branch of iSLN:
- laryngeal surface of the epiglottis
- pyriform recess
Middle branch of iSLN:
- aryepiglottic folds
- False (ventricular) folds
- True vocal folds
Inferior branch of iSLN:
- arytenoids
- proximal subglottis
- posterior glottic wall (interarytenoid space)
- upper esophageal sphincter
Figure 2 of their 2021 article shows where the sensation is the most intense to elicit a bilateral laryngeal adductor response (i.e., the LAR, which is a protective rapid vocal cord closure response to airway invasion).
The afferent nerve density is the highest in the following areas:
- tip of the epiglottis
- false/ventricular folds,
- arytenoids,
- interarytenoid space, and
- posterior glottic wall.
- Whereas sensation to the true vocal cords themselves have less afferent nerve density (from the middle iSLN). There is no LAR response along the membranous portion of the true vocal folds.
I must reiterate that:
There is much more density of sensory nerve fibers above the vocal cords (highest at the epiglottis, aryepiglottic folds, interarytenoid space and all supraglottic spaces) versus at the true vocal cords themselves.
Sinclair, et al 2017 also found that bilateral LAR responses were almost absent in the true vocal folds, as well as the immediate subglottis and epiglottic petiole. Thibeault’s discussion and article (Foote & Thibeault, 2021) reviewed this work.
It seemed shocking to me that the vocal folds lack an LAR response. However, Dr. Thibeault noted that this may be due to the need to distribute fibers in humans more broadly, as humans use the true vocal cords for many other functions, such as during swallowing, phonation (talking) and throat clearing/coughing (Foote & Thibeault, 2021). There is more to this story…
What are TRPV 3 & 4
Dr. Thibeault’s lab investigates the transient receptor potential vanilloid or TRPV 3 & 4. These are proteins that are ion channels in cell membranes that allow ions to pass through. There are a total of at least 28 different types of TRPV ion channels, responding to pressure, heat, chemical sensations. Interestingly, Jetté et al. (2020) found that there are TRPV 3 & 4 taste receptors on the arytenoid cartilages!
Thibeault’s lab found:
“At the region of the vocal folds, there is very limited expression” of TRPV 3 & 4
versus the more robust distribution in the anterior glottis, arytenoids, and epiglottis (in a mouse model). These mouse models are similar to humans; there are not many TRPV receptors on the vocal folds themselves, versus the more robust representation in the subglottis and supraglottis.
Per Thibeault: TRPV (aka, TRPV3/4) chemoreceptors are thought to play a large role in airway protection from fetus through the lifespan. They can trigger glottic closure and apnea in a newborn and a cough reflex later in life. There are “hot spots,” per Thibeault, that are mainly in the supraglottis, epiglottis, aryepiglottic folds, mucosa around the arytenoids, and in the subglottic tracheal epithelium. The posterior supraglottic region is particularly robust with these chemoreceptors and mechanoreceptors. This rich sensory environment ABOVE the vocal folds signals the need to eject material away from the airway. These pharyngeal and laryngeal hot spots carry out a “mucosal surveillance” per Foote and colleagues, 2022 (page 1971). Whereas the vocal folds themselves have minimal receptors. Development of these sensory receptors during pre- and peri-natal development is essential to protect the airway and carryout the complex sequence that is normal swallowing.
Dr. Thibeault noted that there are rapidly responding/rapidly adapting (R1) ion channels and slowly adapting (R2) types:
- R1 = triggers rapid ipsilateral thyroarytenoid response 15-18 milliseconds after the stimulus
- R2 = triggers a delayed but independent bilateral thyroarytenoid response 60-70 milliseconds after the stimulus.
We may expect a response to residue in lower pharynx and to penetration into the upper larynx, but these responses may then adapt quickly. What if the first response is not detected by the clinician on the instrumental examination, and then the subsequent responses diminish as the system quickly habituates? In other words, maybe new responses are no longer re-elicited in a robust way that is detectable by the clinician on an examination. The clinician would have to ask themselves: did I miss the person’s protective response and/or are they unable to detect and trigger another response to new invasions?
Clinical Problems & More Questions
This may create a problem with how we view airway invasion events with the Penetration-Aspiration Scale (PAS; Rosenbek et al., 1996). Penetration into the top of the laryngeal vestibule is rated as a PAS score of 2 when it is completely ejected, and this is completely within normal limits. This sensory research highlights that sensing and ejecting material in the supraglottic space is normal and to not label is as an aspiration risk or dysphagia. Whereas, when material is still above the level of the true vocal cords and not ejected, that is abnormal and rated as a PAS of 3. The PAS does not ask if the person tried to eject, and I would suggest that this would be important information if the clinician can make that judgement accurately. Per this sensory research, one would expect a response when the penetrated material is within this sensory rich environment. However, we need more research to tell us what that response really should be (e.g., just another swallow or a throat clear/cough). Additionally, what if the penetration keeps happening? Is it normal to have a lack of response to repeated penetrations within a short period of time?
A PAS of 4 is quite rare, as that is when the material contacts the vocal cords and is ejected from the airway. This research shows us why that is so rare. When the penetration is to the level of the vocal cords and not ejected, it is rated as a PAS of 5. That tends to make us worry that aspiration is eminent. However, are we expecting too much out of the true vocal cords? Did that drip of liquid fall directly to the true vocal cords where one would not expect an LAR response? This research would suggest that an ejecting cough response may not be seen, since the vocal cords themselves do not have rich sensory receptors. Therefore, is a PAS of 3 just as bad as a PAS of 5? These questions further highlight how the PAS is really more descriptive and not at all an ordinal scale (where the order matters in the amount of severity), as discussed by Steele & Grace-Martin (2017).
We are generating more questions and have more need for research than we have answers. The research is not yet abundant enough yet to change the PAS. But, the clinician may need to ask themselves: did I miss the protective response and are they unable to detect and trigger another response to new invasions? Is this person missing these “hot spots” of sensation that are above the true vocal cords themselves, or are there so many penetration events that their larynx is desensitized?
In further discussion after the conference with Dr. Catriona Steele, Ph.D., CCC-SLP, S-LP(C), Reg. CASLPO, ASHA Fellow (and now current DRS President 2024-2025), she summarized this challenge as:
“The information that I found MOST intriguing was the idea that once those sensory receptors have been excited, there may be a latency during which they cannot re-fire – and as such, once material is in/near the laryngeal vestibule (larynx) and has, for want of a better term, attracted the attention of those receptors, then they may be unable to notice or respond to the arrival of new-additional material.”
Another question and/or problem I see is: What should the response be to penetration? Typically, experts have advised that a cough response is not expected with only a penetration event (i.e., when penetrated material is within the supraglottic space – above the level of the vocal cords). Experts have advised against using the term “silent penetration,” as one should only expect a dry swallow response to penetrations. Dr. Catriona Steele commented during this session’s Question & Answer period that this idea of eliciting a swallow response had come mostly from animal research, as noted in her review article with Dr. Art Miller in 2010. However, that Steel & Miller (2010) article was “a review of sensory input pathways and mechanisms” and discussed stimulating pharyngeal swallowing with a variety of sensory inputs. This article did not fully review the elicitation of a cough based on hypopharyngeal post-swallow residue and laryngeal penetration above and to the vocal cords.
Per that prior advice to not use the distinction of silent versus overt when describing penetration, one should only expect an overt sign of an ejecting throat clear or cough when material hits the vocal cords or drops below the vocal cords. The terminology of silent aspiration has been acceptable and can be considered abnormal. However, given that the supraglottic region has more robust sensory receptors than the true vocal cords and immediate subglottic space, that prior advice may be too simplistic. Per the above sensory research reviewed by Dr. Thibeault, it seems dysphagia evaluations should expect a response when food/liquid or other material is remaining after the swallow near the tip of the epiglottis or near the arytenoids (e.g., in the pyriforms). This is referred to as residue in the hypopharynx. One may also expect a more robust sensory response to material penetrating into the top of the larynx (i.e., in the supraglottic space of the laryngeal vestibule) to the false vocal folds or falling in posteriorly from the pyriforms into the interarytenoid space and posterior glottis? We simply do not know what type of response we are expecting to these penetrations. That response may be a variety of more silent versus audible events, such as a dry swallow, an exhalation, a throat clear, or a more robust cough response.
Bottom line on sensation and airway protection:
The larynx should sense the airway invasion and trigger reflexive responses to eject when the material is still above the vocal folds.
Connecting the Dots to Show Why DRS
DRS is also a wonderful opportunity to start connecting the dots! A poster at DRS seemed to reinforce these pharyngeal and laryngeal “hot spots” that carry out a “mucosal surveillance” (as described by Dr. Thibeault). Katy Anderson, Therese O’Neill Pirozzi, and Joan Kelly Arsenault presented a poster titled: What’s Coughing Got to Do With It?. They studied a large number of patients who were referred solely because of a cough – for Modified Barium Swallow Studies through MassTex Imaging, LLC (MBSS, aka, VFSS/Videofluoroscopic Swallow Studies). They noted that the referral due to a presence of a cough alone was not associated with actual aspiration on the study. Interestingly though, it was associated with the presence of pharyngeal residue and inadequate clearance of this residue. This is interesting in light of the above information on rich sensory environment in the hypopharynx and supraglottic space. The researchers stressed the importance of instrumental examinations.
Can we also make the thought leap to question if those people were coughing in response to frequent residue, protecting their airway with frequent coughing throughout a meal?
This lends itself to our thought in the dysphagia field that coughing is a good and protective sign and NOT a sure sign of aspiration. I must note here that this highlights another benefit of DRS in that it fosters collaboration across the clinician — researcher gap. This was clinician-lead with Andersson and Arsenault collaborating with Dr. O’Neill-Pirozzi, a Northeastern University professor/researcher.
More Discussions & More Research Needed
Discussions and time for Questions & Answers are so helpful to process what we are hearing. We always need more of time to DIGEST the abundant information at DRS. I will attempt here to capture a bit of our discussion from after this session, moderated by Alicia Vose, PhD, CCC-SLP.
Dr. Catriona Steele summarized during the Q&A and afterwards that she still feels uncertain about the term “silent penetration,” as it is unclear whether the penetration would really be expected to trigger an audible cough versus just a dry swallow or other responses. Dr. Thibeault and Dr. Dion both answered that they would expect to see an actual cough in response to penetration where the density of the fibers are higher above the vocal folds. Dr. Dion noted this uncertainty with the label may be in how we have used the term “silent.” If the did response occur, but the material stays in the larynx, “you are not allowing those reflexes to repolarize.” Therefore, you will not see repeated ejection attempts. Dr. Steele commented that “there is a latency here that we don’t factor in” to our evaluation ratings.
Dr. Thibeault answered a question about sensory testing with FEES that had been coined FEESST by Dr. Jonathan Aviv & colleagues (1998) in the past, stating that this had not been a validated measure and has fallen out of favor. It is hard to measure how closely or strongly an air puff gets to what tissue.
Dr. Brittany Krekeler (University of Cincinnati) questioned what happens in chronic aspirators if the mechanoreceptors adapt rapidly and desensitize rapidly. Dr. Thibeault reassured us a bit when she noted that she was talking about mechanoreceptors that are ion channels, which are the ones that adapt quickly (open and close quickly) and may become desensitized to repeated airway invasions. However, there are other mechanoreceptors that are more slowly adapting. Krekeler also wondered at what level is the breakdown when there is poor sensation in a person with a stroke? What is the mechanism of improvement? Is it at the level of the receptors, peripherally in the nerves, or cortically – or – more likely in the integration and reorganization of all levels? Krekeler also encouraged stimulation of sensation with varying tastes and textures of foods/drinks too, as was our first session of this pre-conference day.
We heard from Dr. Greg R. Dion, MD, FACS during this laryngeal reflexes panel and afterwards in the Q&A. He agreed that from a clinical standpoint, you want those protective reflexes to be elicited when the material is still above the vocal cords. He agreed that would make the most sense, as the highest density is in the epiglottis, false vocal folds and the inner arytenoid space.
Dr. Greg Dion continued the laryngeal reflexes discussion with interesting teaching on how we need airflow through the trachea and larynx to stimulate mechanoreceptors in order to help with the swallow response. He stressed the importance of cuff deflation on trachs, even slightly, to increase airflow and increase clearance on cough. People who have tracheostomies with no supraglottic airflow will have worse clearance, swallowing, and cough. Significant subglottic stenosis (severe airway narrowing below the level of the vocal cords) will prevent people from tolerating a speaking valve, which requires airflow above the level of the trach and through the vocal cords. For those who cannot tolerate a speaking valve to restore airflow, he encouraged this idea of digging deeper and asking what else can be done to restore this sensation to the larynx and upper airway. He has made customized trachs with fenestrations or used Montgomery T-tubes to cross over the stenotic region.
Another audience member asked if respiratory strength training (e.g., EMST) could improve sensation and airway sensitivity. While not actually training sensation, the clinician has observed that after a program of EMST, some people seem to better sense residue and airway invasion. Dr. Dion noted that this makes sense if EMST is working on the whole realm of cough. Working the cough will work the false vocal cords too, which as they come together, they will allow you to build up better subglottal pressure. That will in turn help stimulate stronger glottal closure. Overall, there is a stimulation of airflow, which will stimulate more mechanoreceptors.
Summary of Why DRS:
This #1 Why DRS highlight brought up so much more than simply the need to keep questioning. DRS also assists with key needs within the field of dysphagia: constant continuing education, focusing in on our questions that require more research, more interdisciplinary/transdisciplinary discussions, and the bridging of the “gap” between clinicians and researchers.
This #1 Why DRS taught us more about sensation, which is crucial. We forget about sensation. The dysphagia clinician describes the movement and timing of the swallow or what the ball of food/liquid (bolus) does as it moves through the mouth, throat, and into the esophagus. However, the safety and efficiency of someone’s swallow first depends on sensation. Sensory input triggers these good/timely motor movements, but we then depend on an intact sensory system for clearance of any residue or penetration and aspiration.
Finally, the phrases coined by Dr. Thibeault and her team of:
- hot spots
- mucosal surveillance
are very useful and will aid in our future discussions and discoveries. We are just starting to understand sensory swallowing issues.
Dr. Jesse Hoffmeister, PhD, CCC-SLP (also a panelist) had a statement in his talk that applies well to this #1 Why DRS section:
“Unexpected findings driving science forward…”
*******
I hope you will also share your highlights from DRS this year and other years. See my prior DRS Digest blogs here that continue to answer the question of Why DRS:
- DRS Digest (News from Dysphagia Research Society 2016)
- DRS Digest 2017: Raising Awareness through Research
- DRS Dysphagia Digest 2018 (Part 1)
- DRS Dysphagia Digest 2018 (Part 2)
- Dysphagia Digest (Part 3): What is in Your Dysphagia Toolbox?
- DRS Digest: 6 Summaries of Parkinson’s Disease Research
- Dysphagia Digest: Multiphase Dysphagia Evaluations
References:
Aviv, J. E., Kim, T., Thomson, J. E., Sunshine, S., Kaplan, S., & Close, L. G. (1998). Fiberoptic endoscopic evaluation of swallowing with sensory testing (FEESST) in healthy controls. Dysphagia, 13(2), 87–92. https://doi.org/10.1007/PL00009561
Foote, A. G., & Thibeault, S. L. (2021). Sensory Innervation of the Larynx and the Search for Mucosal Mechanoreceptors. Journal of speech, language, and hearing research: JSLHR, 64(2), 371–391. https://doi.org/10.1044/2020_JSLHR-20-00350
Foote, A. G., Tibbetts, J., Bartley, S. M., & Thibeault, S. L. (2022). Localization of TRPV3/4 and PIEZO1/2 sensory receptors in murine and human larynges. Laryngoscope investigative otolaryngology, 7(6), 1963–1972. https://doi.org/10.1002/lio2.968
Jetté, M. E., Clary, M. S., Prager, J. D., & Finger, T. E. (2020). Chemical receptors of the arytenoid: A comparison of human and mouse. The Laryngoscope, 130(2), 423–430. https://doi.org/10.1002/lary.27931
Rosenbek, J. C., Robbins, J. A., Roecker, E. B., Coyle, J. L., & Wood, J. L. (1996). A penetration-aspiration scale. Dysphagia, 11(2), 93–98. https://doi.org/10.1007/BF00417897
Steele, C. M., & Miller, A. J. (2010). Sensory input pathways and mechanisms in swallowing: a review. Dysphagia, 25(4), 323–333. https://doi.org/10.1007/s00455-010-9301-5
Steele, C. M., & Grace-Martin, K. (2017). Reflections on Clinical and Statistical Use of the Penetration-Aspiration Scale. Dysphagia, 32(5), 601–616. https://doi.org/10.1007/s00455-017-9809-z
Note: true vocal cords (TVC) and vocal folds are used interchangeably


I’ve been visiting this site for years, and it never fails to impress me with its fresh perspectives and wealth of knowledge. The attention to detail and commitment to quality is evident. This is a true asset for anyone seeking to learn and grow.
The breadth of knowledge compiled on this website is astounding. Every article is a well-crafted masterpiece brimming with insights. I’m grateful to have discovered such a rich educational resource. You’ve gained a lifelong fan!
I so enjoy reading your blog and its depth of clinical reasoning. Its reinforcement of both being a lifelong learner and the critical importance of having more questions than answers . You are amazing. As a pediatric specialist, I find multiple applications to my clinical practice and teaching. Thank you!
Thank you so much!!
Please let me know if you would like to contribute a pediatric dysphagia blog?
Sincerely,
Karen of SwallowStudy.com and SwallowStudy & Associates, LLC